Danger Week
On ADHD, PMDD, and the 216 cycles it took to understand my own body and mind
Author’s Note:
This piece draws on my own lived experience of PMDD, ADHD, and Autism, diagnoses that arrived late, one by one, and each time changed how I understood my own history. I am not a medical professional. What I share here is personal testimony, supported by research I encountered and sought out largely on my own. If any of it sounds like your story, I hope it offers what it gave me in that conference room in Amsterdam: a name, and the knowledge that you are not crazy.
Trigger warning:
This piece discusses premenstrual dysphoric disorder (PMDD), late diagnosis, and suicidal ideation, including statistics on suicide risk in people with PMDD and ADHD. Please read with care if these topics are close to home.
If you are struggling, you are not alone, and you don’t have to keep searching for answers on your own. If you are in crisis, please reach out to the 113 Suicide Prevention helpline in the Netherlands or the Crisis Text Line in your country.
The slide that changed everything
I eagerly got off the metro at Amsterdam RAI on a random Sunday afternoon in May 2023 to attend the 9th World Congress on ADHD. As I reached the dimly lit conference room, a quick scan of my surroundings was all it took for my anxiety to kick in, realizing that yet again, I was the only Black woman in the room.
Still, I sat there, amongst parents, neurokin, and scholars, steadfast in my quest for answers about my ADHD for the sake of my mental and physical health. I wasn’t too sure what to expect from this special-for-the-public day organized by a Dutch advocacy organization for people with ADHD, but I just knew I had to be there.
Professor Sandra Kooij.
I recognized her name from my post-diagnosis deep dives into my condition. She was there to speak of ADHD in women, particularly on the condition’s relationship with our hormonal cycle.
I got really excited to hear her speak until…
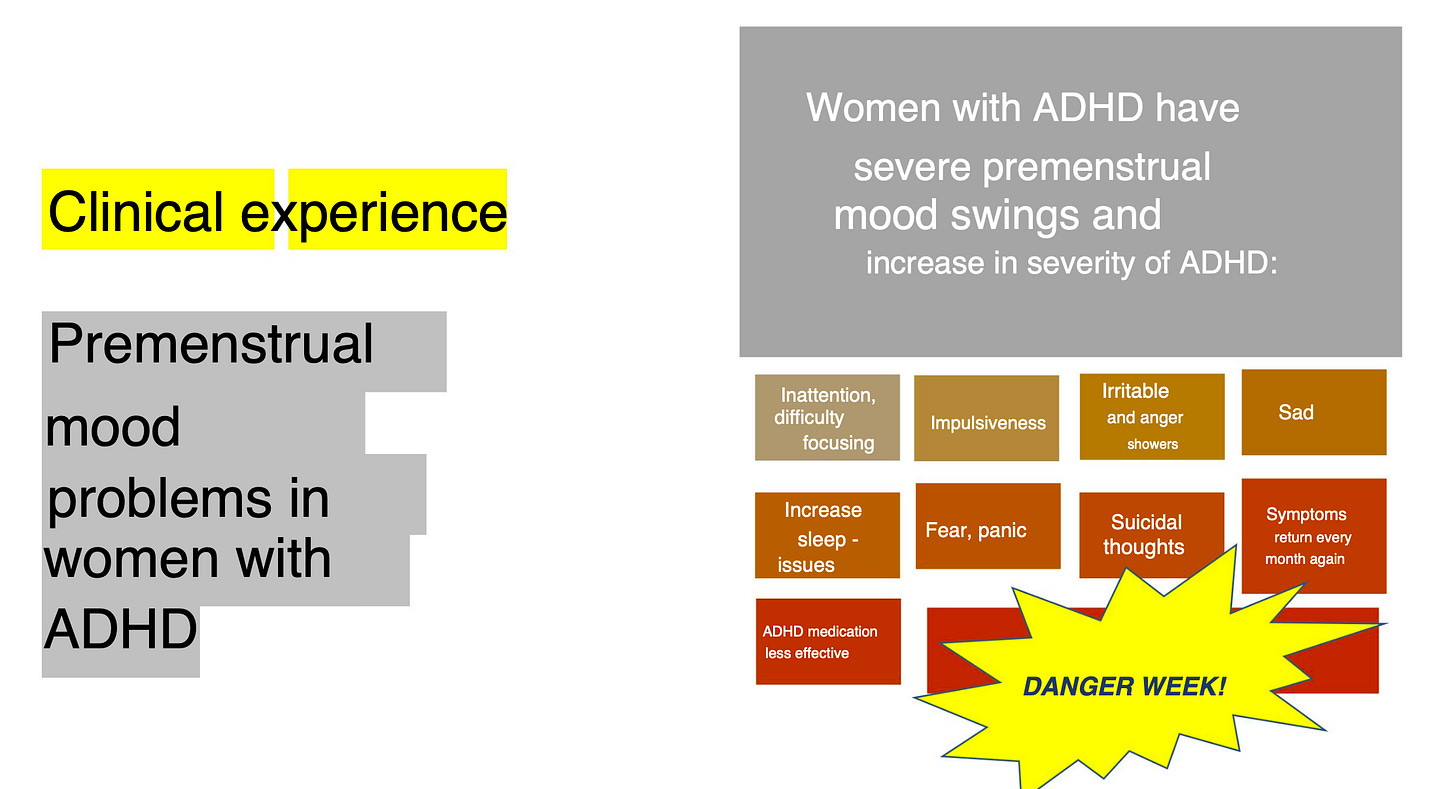
“DANGER WEEK.”
There it was, written in yellow.
My heart started beating faster as Professor Kooij started describing the increase in severity of mood swings in the premenstrual phase of women with ADHD’s cycle.
“She’s speaking of me”, I immediately thought. And “I am not crazy.”
There was an explanation for the monthly psychological torment I go through, and she was calling it PMDD.
Premenstrual dysphoric disorder.
A condition characterized by brain fog, severe irritability, rage, sadness or depression, during the menstrual cycle. Basically, premenstrual syndrome (PMS) squared, or on steroids, as I often like to joke about.
As she went further into her presentation, it quickly became clearer why this condition, affecting only about 5% of people who menstruate, shows up in nearly 45% of women with ADHD.
Estrogen, a primarily female sex hormone crucial in the regulation of our menstrual cycle, rises and falls in ways that directly impact dopamine, a critical neurotransmitter responsible for motivation, focus, pleasure, and that fragile ability to just… get started on things, which is already dysregulated in people with ADHD.
My ADHD makes the experience of my menstrual cycle worse. And, the other way around.
“For Christ’s sake! When does one get respite?”, I thought to myself as a complex cocktail of emotions started bubbling up in me.
Though I wasn't officially diagnosed with PMDD until I sought my Autism diagnosis, nearly two years after my ADHD assessment, I knew deep in my gut that this woman was describing, and most importantly, naming much of my experience to a T.
PMDD, another medallion in the collection of delayed answers, diagnoses, I had to fight for, trickling down one by one, three decades in.
There was a bittersweetness to gaining this extra set of keys to my brain and body.
Professor Kooij tried to alleviate the atmosphere by making jokes about women's testimony of the cyclical rage their partners had to “endure”. A rage capable of turning us into some kind of monsters that had to be handled with extra care on PMDD days.
Two hundred and sixteen
I, too, laughed, but the relief I felt was juxtaposed with incomprehension, a sense of injustice, and profound grief at receiving this information only at 30. 216 menstrual cycles if I round it up.
216 cycles, where I didn’t understand what the hell was going on with me.
216 cycles where my recurrent suicidal thoughts nearly took the best of me, because life suddenly felt somber, tasteless, and unbearably heavy.
216 cycles where the irritability-to-rage pipeline I experienced, triggered by interactions with others and my inner world, often internalized, sometimes externalized, damaged, or cost me relationships with family members, friends, and partners.
216 times where I felt like a prisoner in my own body for up to two weeks in a month.
The labour of knowing
Until that Sunday in May 2023, not being able to explain my PMDD experience to others had left me profoundly alone with it.
As I did not know what was actually happening to my body, I’d been led to believe I was just experiencing regular PMS, like most women do. Nothing to see here, move along type of experience. I had no label for it and not the faintest idea it could be connected to how my brain was wired.
This simply couldn’t just sit with me. I had to do something about it.
As soon as I left the conference center, I reached for my phone to alert others who might recognize themselves in what I had just learned, through these facts & figures on my Instagram stories.
At home, my ex-partner looked at me in confusion as I told them I was adding yet another condition to the list and that this one might actually explain some of the hardest moments in our relationship, particularly after ovulation.
A couple of weeks later, I went to my general practitioner (GP), as advised by Professor Kooij, to ask for an increase in my ADHD medication during my luteal phase — the two weeks before my period, when PMDD takes hold.
The female GP looked at me with the same perplexed expression my partner had worn days before, as I shared the information I had received from her peers at the conference.
There I was again, having to educate someone with far more medical training than I that my hormonal cycle affects my ADHD. My self-advocacy for better treatment made me share Professor Kooij’s slides, just to be taken seriously. To secure, as I came to think of it, a semblance of care.
After a couple of days waiting, my request was approved, and I started receiving an increased dose of my ADHD medication for 10 days each month.
Getting the medication was not the end of my struggle.
In true ADHD style, applying what I know best for me and how it actually plays out remains a challenge and a half. My brain experiences executive dysfunction, making it all the harder to self-manage through routines and impulse control, to remember simple to-dos like taking your meds, or to defeat binge eating or doomscrolling late at night.
A cruel irony, if you ask me. The very brain making my life more challenging was also the one standing between me and the things that could make it easier.
Over time, it became clear that medication alone wouldn’t be enough. In fact, I had to become more conscious of the importance of sleeping sufficiently, mindfulness, adapting my diet, and exercising as ways to manage these symptoms. I later found out that certain herbal teas and vitamin or plant-based supplements, even acupuncture, could be remedies for managing PMDD and easing our lives. Most of this additional information I had to find myself, through research articles and others’ lived experiences online. It wasn’t provided by my healthcare practitioners, even by the ones who diagnosed me.
The weight we carry
One thing was clear: if I was only finding out this late into my adult life, who was going to help the thousands, heck, millions of women and other menstruators walking through their doctors' offices seeking answers they might never get because the medical scholars and practitioners were still stuck in the 90s, armed with outdated, often sexist understanding of ADHD in women and women’s health, full stop.
Whether for endometriosis or ADHD, women continue to be misdiagnosed, underdiagnosed, or simply missed by the very systems meant to care for them.
The cost is not abstract: 72% of people with confirmed PMDD have experienced suicidal ideation in their lifetime, and 34% have attempted suicide (Eisenlohr-Moul et al., 2022). Among women with ADHD, suicide attempts are already seven times more likely than in women without it — with 23.5% of women with ADHD having attempted suicide compared to just 3.3% of women without — driven largely by the co-occurring anxiety and depression that PMDD only compounds (Constance, 2021).
Many of our lives are in crisis, and I still hear people making silly comments about ADHD being overdiagnosed these days or joking that “everyone is a little ADHD”, making me want to scream. It is infuriating that people are ignorant of how these health inequities and negligence are costing people’s lives.
The awareness I gained about these manageable conditions has been so life-changing that I committed to sharing what I had learned with friends, on social media, and even during my neurodiversity keynotes and workshops for my various clients. No matter how little or big my reach might be.
But there’s no amount of explaining, stating facts, and finger-pointing that could fully paint a picture of the lived experience of ADHD-PMDDers’ hormonal cycle.
Still, it is urgent that we, those with lived experiences, dump the taboos and find the courage to openly speak up about our experiences, for we may not fully measure how many lives the ripple effect of telling the truth is literally saving.
What has been equally hard to accept is how ADHDers affected by this combo of hell are systemically disempowered to fully participate in society. We carry a heavier mental load, with our disabilities’ symptoms endlessly fluctuating throughout the month and at different stages of our lives.
And yet we are still expected to keep going to work, to pay the bills, to perform our daily tasks, to manage the traditional household, to take care of children, and to take care of ourselves, with the same ease as others.
The invisibility of our conditions doesn’t make them any less real. It is a true disability that deserves the full range of accommodations in schools, at work, in the private and public spheres, as any other disability or impairment.
It shouldn’t get to the point of us creating a PMDD simulator or VR experience, as we've done with our periods, for others to take us seriously and support us.
Society still hasn’t caught up, and it forces me to work twice as hard to exist in a body and mind that is fatigued. As if being a woman, a Black woman, isn’t already hard enough in itself.
I think of my grandmother, who was undiagnosed before she left this earth, but displayed many signs of ADHD. And of my own mother, battling menopause with an ADHD brain — how no matter how I tell her the role of hormonal fluctuations in women with ADHD, she remains undiagnosed, untreated, and unsupported. No matter how I share how her symptoms could be alleviated if her ADHD was factored into managing the fatigue, severe irritability, or difficulty sleeping she's been dealing with lately.
Generations and generations of menstruators, our patriarchal society has neglected, one after another. I can only imagine how my mother, her mother, and my grandmother’s mother would have benefited from the knowledge I will share with my children when the time comes.
This is why I was relieved to hear that the preliminary results of Professor Kooij’s research, the research that changed the course of my life, have since been published in November 2025, confirming that hormonal fluctuations exacerbate ADHD symptoms and mood disturbances, and highlighting the vulnerability of undiagnosed ADHDers to PMDD, postpartum depression, and cardiovascular disease during perimenopause.
Beyond borders
Whilst these scientific findings are a turning point for women’s health, I hope that their translation into medical practice accelerates the saving of lives, beyond the borders of the West, where women facing these challenges are far less informed, supported, and cared for.
I think of my home country, Benin, where psychological support of mental health disorders remains fragmented and privileged; many moving from therapist to therapist, across both traditional and Western practices, in search of answers. Far more women are carrying the weight of undiagnosed ADHD, unnamed PMDD, or both, without the language, access, or research to make sense of their own bodies.
They should not be an afterthought.
As more of us speak up about the weight of our lives, may our voices reach those still lost at sea:
For my grandmother, who never got the words.
For my mother, who still doesn't have them.
And for every woman still searching, I hope this finds you before another 216 cycles pass.
References
Constance, L. (2021, January 5). Study: Nearly one in four women with ADHD has attempted suicide. ADDitude Magazine. https://www.additudemag.com/adhd-in-women-suicide-risk/
Eisenlohr-Moul, T., Divine, M., Schmalenberger, K., Murphy, L., Buchert, B., Wagner-Schuman, M., Kania, A., Raja, S., Miller, A. B., Barone, J., & Ross, J. (2022). Prevalence of lifetime self-injurious thoughts and behaviors in a global sample of 599 patients reporting prospectively confirmed diagnosis with premenstrual dysphoric disorder. BMC Psychiatry, 22, 199. https://doi.org/10.1186/s12888-022-03851-0
Kinoo, P. (n.d.). Valeur Vodun ou la famille restructurée. Retrieved from https://www.philippekinoo.be/enfants-vulnerables-et-ethnopsychiatrie/12-valeur-vodun-ou-la-famille-restructuree
Schmalenberger, K., & Kooij, S. (2025). Hormonal transitions and ADHD in women. Frontiers in Global Women’s Health. https://www.frontiersin.org/journals/global-womens-health/articles/10.3389/fgwh.2025.1613628/full
© Axelle Ahanhanzo, 2026. Please do not reproduce without permission and attribution.


